What are the noticeable signs of acute kidney injury? Spotting renal damage isn’t easy, but early detection is vital.
Kidney Injury
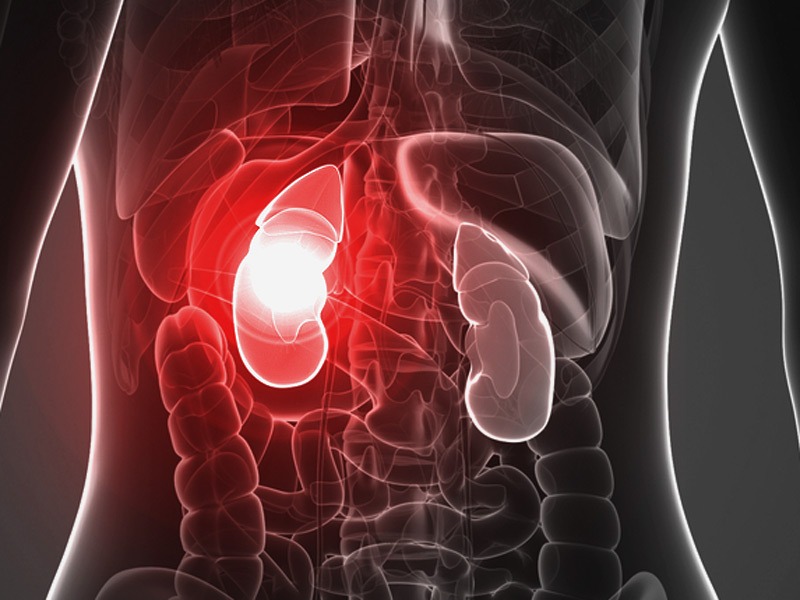
Acute kidney injury (AKI), also known as acute renal failure, occurs when the kidneys are suddenly unable to filter waste products from the blood. When this happens, dangerous levels of waste products such as creatinine and blood urea nitrogen (BUN) may accumulate, leading to even more dangerous conditions such as sepsis. To combat this, it is vitally important for physicians to quickly identify the signs and symptoms of AKI before it has a chance to progress.
There are many different reasons why a patient may develop AKI, but the three overarching themes are typically: decreased blood flow to the kidneys, direct damage to the kidneys, and blockage of the urinary tract. Let’s examine each one individually.
Decreased Blood Flow: Some of the most common causes of AKI include hypotension and hypovolemia. Similarly, any condition that affects the heart’s ability to circulate blood throughout the body – such as recent surgery, burns, NSAIDS, and organ failure – are attributing factors to AKI.
Direct Damage to Kidneys: Diseases and conditions that damage your kidneys are often causative factors of acute renal failure. Some of these conditions include sepsis, multiple myeloma, vasculitis, and glomerulonephritis.
Blockage of the Urinary Tract: In some cases, the blocking of the urinary tract can lead to renal insufficiency. These blockages can be caused by several factors, including bladder cancer, enlarged prostate, kidney stones, and blot clots in the urinary tract.
Reference: https://www.asn-online.org/
Spotting AKI Before It Progresses
Early detection of AKI is vital and could mean the difference between life and death for a patient. When talking about early detection, most physicians will reference urine output as the “gold standard” of kidney function. While this is certainly a reliable method of gauging the efficiency of the kidneys, there are other ways to detect AKI as well.
Some symptoms of AKI include confusion, nausea, fatigue, and chest pain. Although these symptoms could be correlated to several conditions, they are important for indicating AKI because they occur in the early stages before the damage to the kidneys has progressed significantly.
Reference: https://jasn.asnjournals.org/
Courtesy of KDIGO
It is also recommended to manage patients according to their susceptibilities and exposures to reduce the risk of AKI (see relevant guideline sections).
Most notably, KDIGO suggests testing patients at increased risk for AKI with measurements of SCr and urine output to detect AKI.
Renal Insufficiency – Getting Tested

If a physician suspects their patient has AKI, there are a few tests they may perform to get additional information on the function of the kidney. Traditionally, the most reliable test is continuous monitoring of urine output, as urine production is arguably the most accurate measurement of kidney function.
However, since the kidney also serves to filter waste products from the blood stream, many physicians will opt to test the blood of the patient and evaluate the levels of creatinine, BUN, and potassium. A blood draw can also be used to perform a test of glomerular filtration rate (GFR), which is used to estimate the decrease in kidney function for patients suspected of acute renal failure.
In more severe cases, a physician may order a variety of imaging tests, such as an ultrasound or CT scan, to look for any abnormal signs of renal insufficiency. If the images reveal no additional information but the physician still suspects AKI, it is possible he/she will order a biopsy of the kidney for further evaluation by pathologists.
Reference: https://www.healthline.com/health/kidney-function-tests#types
Renal Failure – Signs And Symptoms
When AKI is not detected early enough and allowed to progress, it becomes known as chronic kidney disease (CKD) or renal failure. There are 5 stages of CKD, all associated with a specific range of eGFR. Unfortunately, once the damage to the kidneys has reached a point where it is considered CKD, there is little that can be done to reverse the damage.
| Stage | eGFR Values | Note |
| 1 | normal or high GFR (GFR > 90 mL/min) | There are usually no symptoms to indicate the kidneys are damaged. Because kidneys do a good job even when they’re not functioning at 100 percent, most people will not know they have stage 1 CKD. If they do find out they’re in stage 1, it’s usually because they were being tested for another condition such as diabetes or high blood pressure (the two leading causes of kidney disease). |
| 2 | Mild CKD (GFR = 60-89 mL/min) | There are usually no symptoms to indicate the kidneys are damaged. Because kidneys do a good job even when they’re not functioning at 100 percent, most people will not know they have stage 2 CKD. If they do find out they’re in stage 2, it’s usually because they were being tested for another condition such as diabetes or high blood pressure–the two leading causes of kidney disease. |
| 3A | Moderate CKD (GFR = 45-59 mL/min) | This stage is broken up into two: a decrease in glomerular filtration rate (GFR) for Stage 3A is 45-59 mL/min and a decrease in GFR for Stage 3B is 30-44 mL/min. As kidney function declines waste products can build up in the blood causing a condition known as “uremia.” In stage 3 a person is more likely to develop complications of kidney disease such as high blood pressure, anemia (a shortage of red blood cells) and/or early bone disease. |
| 3B | Moderate CKD (GFR = 30-44 mL/min) | This stage is broken up into two: a decrease in glomerular filtration rate (GFR) for Stage 3A is 45-59 mL/min and a decrease in GFR for Stage 3B is 30-44 mL/min. As kidney function declines waste products can build up in the blood causing a condition known as “uremia.” In stage 3 a person is more likely to develop complications of kidney disease such as high blood pressure, anemia (a shortage of red blood cells) and/or early bone disease. |
| 4 | Severe CKD (GFR = 15-29 mL/min) | It is likely someone with stage 4 CKD will need dialysis or a kidney transplant in the near future. As kidney function declines, waste products build up in the blood causing a condition known as uremia. In stage 4, a person is likely to develop complications of kidney disease such as high blood pressure, anemia (a shortage of red blood cells), bone disease, heart disease and other cardiovascular diseases. |
| 5 | End Stage CKD (GFR <15 mL/min) | At this advanced stage of kidney disease, the kidneys have lost nearly all their ability to do their job effectively, and eventually dialysis or a kidney transplant is needed to live. |
| KDIGO.Org |
Reference: https://www.davita.com/
Chronic Kidney Disease
For patients living with CKD, the most common measure taken to slow the progression of the disease is a combination of both dialysis and lifestyle changes. In the most extreme cases, however, some patients may undergo kidney transplantation.
For patients making changes to their lifestyle, many have found healthy eating and exercising habits to decrease the negative effects of renal failure. Such changes include making a switch to a low-salt, low-fat and high-protein diet, maintaining healthy blood pressure, reducing alcohol/tobacco consumption, and exercising regularly.
Aside from lifestyle changes, many medications/supplicants have been proven to assist the kidneys in maintaining a working level of functionality. Diuretics have been shown to increase urine production, which eliminates excess salt and water. Additionally, vitamins and dietary supplements are effective at promoting renal function, even in patients who don’t suffer from AKI or CKD.
Reference: http://freseniuskidneycare.com/

